The study and treatment of cancer remain at the forefront of modern medical science. Representing a broad and complex category of over one hundred distinct diseases, this condition fundamentally stems from the uncontrolled proliferation of abnormal cells. While historical perspectives often viewed oncological diagnoses with immense apprehension, contemporary clinical research, advanced diagnostic imaging, and precision medicine have profoundly altered patient prognoses. A comprehensive understanding of cellular pathogenesis, recognizing diverse clinical manifestations, and utilizing state-of-the-art medical infrastructure are essential for optimizing survival rates and enhancing patient quality of life.
The Pathogenesis of Malignancy
At a fundamental biological level, the human body operates through a highly regulated cycle of cellular growth, division, and programmed death, known as apoptosis. This delicate equilibrium is maintained by specific genes: proto-oncogenes, which signal cells to multiply, and tumor suppressor genes, which halt division or initiate cell death when DNA damage is detected.
Malignancy occurs when accumulated genetic mutations disrupt these regulatory pathways. When tumor suppressor genes are inactivated or proto-oncogenes become hyperactive oncogenes, cells bypass natural growth limits. These aberrant cells multiply exponentially, often aggregating to form tissue masses known as tumors. While benign tumors remain confined to their original anatomical site, malignant tumors exhibit aggressive biological behaviors. They stimulate angiogenesis, the formation of new blood vessels to secure an independent blood supply, and they possess the invasive capacity to infiltrate adjacent healthy tissues. Through a process called metastasis, these malignant cells can enter the vascular or lymphatic systems, establishing secondary colonies in distant organs such as the liver, lungs, or skeletal system.
Classification of Oncological Diseases
Medical professionals categorize these diseases based on the specific tissue type from which the abnormal cells originate. Understanding these classifications is crucial for determining appropriate prognostic models and treatment protocols:
- Carcinomas: The most frequently diagnosed category, originating in the epithelial cells that line internal organs and the exterior surface of the body. Examples include adenocarcinoma and squamous cell carcinoma, which often manifest in the breast, lungs, prostate, and colon.
- Sarcomas: Malignancies that develop in mesenchymal tissues, including bone, cartilage, adipose tissue, muscle, and vascular structures.
- Leukemias: Cancers of the blood-forming tissues, particularly the bone marrow. Unlike solid tumors, leukemias result in the overproduction of abnormal, non-functional white blood cells, which overwhelm the circulatory system.
- Lymphomas: Diseases that originate in the lymphatic system, specifically affecting lymphocytes (T-cells or B-cells), compromising the body’s immune defenses.
Etiology and Established Risk Factors
The development of cellular mutations is rarely attributed to a single cause; rather, it is the result of a complex interplay between genetic predispositions and environmental exposures.
Intrinsic risk factors include chronological age, as the likelihood of genetic transcription errors increases over time, and hereditary genetic syndromes. Mutations in genes such as BRCA1, BRCA2, and TP53 significantly elevate the lifetime risk of developing specific malignancies.
Extrinsic or environmental risk factors, known as carcinogens, are critical contributors to DNA damage. Chronic tobacco use remains the leading preventable cause of oncological mortality worldwide, introducing dozens of known chemical carcinogens into the pulmonary system. Prolonged exposure to ionizing radiation, ultraviolet (UV) light, and specific industrial chemicals (such as asbestos and benzene) are heavily implicated in cellular mutation. Furthermore, certain infectious agents, particularly Human Papillomavirus (HPV) and the Hepatitis B and C viruses, are known oncogenic drivers capable of initiating cellular transformation over extended periods.
Clinical Manifestations and Systemic Symptoms
Because this spectrum of diseases can affect virtually any organ system, clinical presentations vary widely. Symptoms are dictated by the tumor’s anatomical location, its rate of growth, and its impact on surrounding structures.
Localized symptoms may include a palpable, indurated mass beneath the skin, persistent changes in bowel or bladder habits, chronic cough, or unexplained hemorrhage. However, malignancies also trigger widespread systemic responses. The rapid metabolic demands of proliferating cells and the immune system’s inflammatory response can lead to cachexia—a severe syndrome characterized by rapid, unexplained weight loss and muscle wasting. Profound fatigue, recurrent fevers, and night sweats are also common systemic indicators that warrant immediate clinical investigation.
Diagnostic Precision and Clinical Staging
Early detection radically transforms the trajectory of patient care. When a patient presents with indicative symptoms, clinicians employ a multifaceted diagnostic approach. Advanced imaging modalities—such as Computed Tomography (CT), Magnetic Resonance Imaging (MRI), and Positron Emission Tomography (PET)—allow for meticulous, cross-sectional visualization of internal physiology, identifying structural anomalies and metastatic spread.
Despite the efficacy of imaging, the definitive diagnosis invariably requires a histopathological examination via a tissue biopsy. Pathologists analyze these cellular samples to confirm malignancy, determine the specific tumor grade, and identify unique molecular markers. Subsequent staging, typically utilizing the internationally recognized TNM (Tumor, Node, Metastasis) system, is imperative. Institutions with advanced diagnostic and multidisciplinary capabilities, such as Liv Hospital, provide the rigorous clinical infrastructure necessary to accurately stage the disease and design personalized therapeutic interventions.
The Evolution of Therapeutic Modalities
Modern oncology has transitioned from generalized treatments to highly individualized, precision medicine. Traditional therapeutic pillars remain foundational: surgical resection aims to physically extirpate localized tumors, while radiation therapy deploys targeted, high-energy ionizing beams to destroy malignant DNA. Systemic chemotherapy utilizes cytotoxic pharmacological agents to eradicate rapidly dividing cells throughout the body.
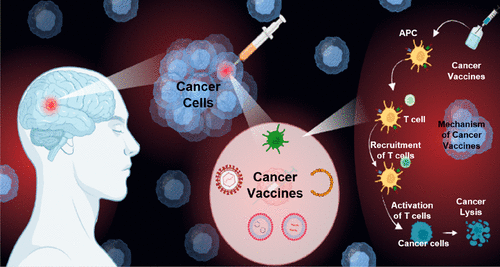
However, recent decades have introduced revolutionary advancements. Targeted therapies are meticulously engineered to interfere with specific molecular pathways or mutant proteins essential for tumor survival, thereby minimizing collateral damage to healthy tissues. Furthermore, immunotherapy has emerged as a groundbreaking paradigm. By utilizing pharmaceutical agents like checkpoint inhibitors, immunotherapy overrides the deceptive signals malignant cells use to evade detection, empowering the patient’s own immune system to recognize and dismantle the disease.
Holistic Well-being and Lifestyle Integration
Beyond the clinical environment, the comprehensive management of complex health conditions demands a profound focus on systemic well-being and physiological resilience. Individuals navigating intensive medical treatments, as well as those focusing on preventative health, benefit immensely from integrating structured lifestyle modifications. Proper nutritional support, characterized by antioxidant-rich diets, alongside adequate hydration and restorative sleep, forms the bedrock of cellular repair and recovery. Mitigating the psychological stress associated with rigorous medical journeys requires a multifaceted approach, often incorporating mindfulness practices and safely tailored physical activity. For individuals seeking authoritative guidance on optimizing daily habits, nurturing mental fortitude, and discovering holistic resources to live and feel their absolute best, an integrated approach to lifestyle medicine offers invaluable support for enduring health and vitality.
Keep an eye for more latest news & updates on Daily Uk!